I'm furious... What. HAPPENED?!?!
- brittanymarkham

- Aug 12, 2022
- 10 min read

August 1st was going to be such a BIG day. I was very nervous: starting a new treatment meant taking the risk of dealing with an allergic reaction, potentially a very severe one, and who knows what kind of hiccups that would throw into our treatment plan.
But I was also thrilled: the timing was impeccable - Damian's liver and spleen have always been enlarged and have progressively been putting pressure on his stomach and lungs, but it was now reaching a pivotal point. Damian's vomiting was definitely increasing and his energy was undoubtedly inhibited by his squished lungs. I had a feeling it was going to really start getting bad from here on out.
Enzyme Replacement Therapy was going to fix all of that - it was going to immediately start shrinking Damian's liver and spleen down to normal size (little by little, over time). It was going to be the 2nd treatment Damian began (in addition to the "Brain 1.0" treatment he started a little over 3 months ago) for his ultra-rare disease. August 1st was such a highly anticipated day.
...Was.
I posted this on Instagram early that evening:
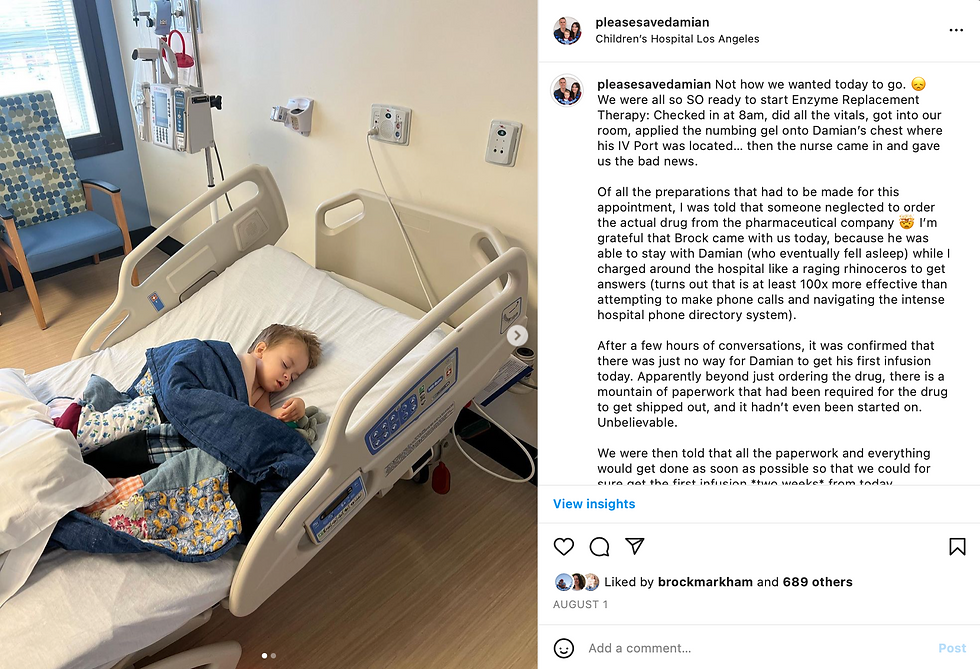
"Not how we wanted today to go. 😞 We were all so SO ready to start Enzyme Replacement Therapy: Checked in at 8am, did all the vitals, got into our room, applied the numbing gel onto Damian’s chest where his IV Port was located… then the nurse came in and gave us the bad news.
Of all the preparations that had to be made for this appointment, I was told that someone neglected to order the actual drug from the pharmaceutical company 🤯 I’m grateful that Brock came with us today, because he was able to stay with Damian (who eventually fell asleep) while I charged around the hospital like a raging rhinoceros to get answers (turns out that is at least 100x more effective than attempting to make phone calls and navigating the intense hospital phone directory system).
After a few hours of conversations, it was confirmed that there was just no way for Damian to get his first infusion today. Apparently beyond just ordering the drug, there is a mountain of paperwork that had been required for the drug to get shipped out, and it hadn’t even been started on. Unbelievable.
We were then told that all the paperwork and everything would get done as soon as possible so that we could for sure get the first infusion *two weeks* from today.
I informed the responsible parties that I would be checking in frequently between now and then to ensure EVERYTHING is squared away and we can actually start treating my son.
Between you and I though, after the conversations I had today, I anticipate a few more hiccups before we’re out of the woods. I’m not even holding my breath for the Aug 15th start date now 💔 I will certainly be following up and pushing for that date, but I’ll also be having some real serious conversations with some people.
Advocating for your child’s health is often difficult and uncomfortable and frustrating. But it’s these types of *very preventable* issues that infuriate me the most. And it happens FAR too often. 😡
BRB. Mama’s gonna do what mama’s gotta do. 🐻"
Many of the messages I received after I posted that echoed perfectly how I felt: incredibly angry and totally mind-boggled knowing that my baby would go even longer without treatment simply due to negligence and incompetence, especially when I had - for months - been asking for confirmation (and was assured every time I asked) from Damian's medical team that we had everything approved and set and ready for an August start date.

However, I said this later that night on Instagram Stories and I'll say it again now: there is certainly a time and a place for venting (and when I need to, Brock is always there to listen, bless him). I do vent. I did vent. But - if I spend more time venting than I spend doing something productive, I will not make progress as quickly as possible. And Damian needs this treatment started as quickly as possible.
So I am not writing this blog post to rant. Instead, I hope explaining what happened and what my response was could benefit someone else who, heaven forbid, is going through something similar.
So WHAT HAPPENED?
That day in the infusion center, I spent a lot of time talking with Damian's "Primary Investigator," which is simply the doctor who agrees to oversee the experimental endeavor (in this case, the Enzyme Replacement Therapy). The conversation we had raised a lot of flags for me, as the doctor's understanding of what needed to be completed in order to get the drug did not at all match my understanding of how a patient gets approved for a clinical trial.
Now, I am not a doctor. I have my masters degree in art and technology for pity sakes. But I have certainly spent a lot of time talking with other parents and professionals currently in this process or who have gone through this process and things just simply weren't sounding logical.
If there is anything that I have learned in the past year and a half of advocating for the health of my child, it's that doctors are very normal human beings that simply studied something different than I did in school. When they are at work they have work to do, and they clock out when they need to go home. Also, not all hospitals are the same - nor are their resources, regulations, and training programs. It is logical to assume that the best health care can be expected by patients with common ailments - where care plans have already been long established and there is no guesswork or critical thinking required by anyone involved.
But we're dealing with a very rare disease. Most doctors have only read about this disease in medical school and will never see a patient with it. Damian is currently the only child with ASMD in the world on this "Brain 1.0" treatment and may very well be the first person ever to be on both the Brain 1.0 and the liver treatment (ERT) at the same time. Our case therefore requires critical thinking, taking initiative in asking questions and seeking out resources, and, very importantly, the ability to create and complete a task list. It doesn't just require medical know-how - it requires communication and managerial skills.
The reason why Damian did not start Enzyme Replacement Therapy on August 1st is because Damian's medical team currently lacks the hospital-equivalent of a project manager.

Unfortunately, no single person was taking responsibility for understanding what tasks needed to be completed and then making sure those tasks got done. When you don't have a captain leading the team, what happens? There is no sense of urgency, no understanding of responsibilities, and things just don't get done.
There is no one in this world that cares about Damian as much as I do. It also turns out that most of my professional career has been in project management, so when the doctor was trying to explain to me why we were sitting on a hospital bed but unable to start the treatment we were scheduled to start that day because he didn't realize that there was still a lot of paperwork to go through, my "spidey-senses" started tingling. I knew this was the tip of the iceberg.
In the past 11 days, I have had many conversations with people from the Clinical Research department, from Damian's doctor's clinical department, and even the executives of the hospital. My conversations with them confirmed that there is a big scope gap that needs to be filled. I was even told that our situation and my involving the upper management (this isn't the first time I've had to pull that card, btw) has led the hospital to start considering a new position for professionals who specialize in initiating and coordinating the care of patients in clinical trials.
I mean... I just... I'm not going to comment on that.
At the very least, there are a lot of eyes on Damian's case now. Let's hope that helps us make up for some serious lost time.
So when WILL the Enzyme Replacement Therapy start?
Incredibly, I am still trying to understand exactly where Damian's enrollment in ERT stands. The story changes slightly with every person I talk to. Very simply put, these are the basic steps to getting started in a normal clinical trial:
The hospital must agree with administering the treatment or therapy there
A doctor has to agree to oversee the care of the patient and meet the demands the trial requires (they become the "Primary Investigator" or "PI")
The PI submits an application on the patient's behalf to the pharmaceutical company or group who is running the trial and owns the drug/treatment
If approved to join the trial, the patient is enrolled and the pharmaceutical company ships the drug to the doctor to begin treatment. The instructions and demands of the pharmaceutical company that must be followed while participating in the trial are called the "protocol."
We are in step 3. I have been told that there are just 3 outstanding forms that will be sent to the pharmaceutical company by the end of today (Friday, August 12th). But because Damian is currently on another experimental drug (the Brain 1.0), the pharmaceutical company may want to treat Damian's trial in a different way or consider making alterations to their protocol and may need to have multiple conversations internally as well as with Damian's doctor and who knows what else - all of which, of course, will delay the approval process.
I don't know when we are going to start the Enzyme Replacement Therapy now. Some people from the hospital are guessing 5-6 weeks. I have no clue how realistic that is. But one thing is for sure: I'll be reminding everyone of the urgency of this and pressing for updates every day. If they're not gonna put a project manager over this case, that role is gonna have to be filled by me. Again.
"Is there anything we can do to help push this along?"

I've had a bunch of people ask me this and I am SO grateful. Thank you so so much!!
Like I mentioned earlier, I have unfortunately had to reach out to the top executives at the hospital before, when we were trying to get the Brain 1.0 treatment started. If anyone can get things moving quickly within the hospital, it's them. They are literally it. They are as high as I can go. And they have been incredibly responsive to me. The fires have been lit (again) and so I don't think a mass amount of emails to them now would be helpful - it may even work against us.
That doesn't mean that that strategy might not become necessary in the future though. So stay tuned.
And I really appreciate anyone wanting to help with issues like this running your ideas past me before contacting anyone else involved :) Thank you so much!!!
Q: How did you get the contact info of the top executives?
A: I guessed at what their emails were. It was easy to find out their names on the hospital's website, and I was able to find on the same website enough emails of other random people to see the pattern of how every email was formatted (i.e. First Initial . Last Name @ _________.com or whatever). The same strategy can be applied to practically every company ever.
I will say this: at this point, the most helpful thing right now is to pray for us that this application can get processed and approved quickly. Damian really needed to start this treatment in August. He seems to have been eating less and less over the past month or two and that really worries me. I mentioned already that he seems to be vomiting more frequently.
I am anxious for him to start this treatment.
Additionally, our ongoing work in spreading awareness and fundraising for the Brain 2.0 treatment is the best action we can take, for two reasons: First, we desperately need to finish the funding portion of our campaign now. A couple weeks ago the key scientist developing the treatment reiterated that funding will make the biggest difference for their research (that and getting plasma samples from ASMD patients).
Secondly, building the community that we are is achieving a lot more than fundraising. It is also opening doors: I had my first magazine interview last week because of you (photos from the shoot below!). I am now able to earn commissions on Amazon (much more lucrative than Amazon Smile, btw) because of you (see our storefront here!). My top-performing Instagram reel, where I introduce Damian and his disease, has reached almost half a million people because of you. And I've always believed that we can do this if we can just reach enough people.
The larger our community is, the more people who care about treating ASMD, the faster our story spreads, the quicker we will get ASMD treated. It is really that simple.
"Is your hospital just awful?"
NO. Absolutely not. I have had a lot of great interactions with people at our Children's Hospital and there are a host of people there that I have literally entrusted with my son's life. Again, I believe when the disease or ailment or procedure you're dealing with is a little more common, there are established precedents and expectations of what needs to be done, people know what resources they have, and so on. You're not as dependent on a very select few knowing how to deal with an extremely rare situation they've probably never dealt with ever. Not to mention that dealing with treatments that are not yet FDA-approved means dealing with a LOT of bureaucracy - and doctors (or anyone else) don't just magically know how to navigate that. That know-how only comes from experience.
I've had a bunch of people suggest that I might want to consider moving, or at least changing hospitals. In certain situations, it's honestly something I've thought about as well. But at the end of the day, so much of this comes down to time. Would the amount of time it would take to do all that be more or less than sticking with our current situation and just pushing and pushing to get that first infusion of ERT? In this moment in time, I think our best bet is to push.
More Updates to Come
I have a feeling there are still a couple hurdles we need to jump to get this ERT finally approved. But I know we will get there, and I'm gonna continue being a raging rhino - hovering helicopter - mama bear manager until we do.
If you haven't already learned this incredibly valuable life lesson, here it is now: the squeaky wheel is the one that gets greased.
Stay squeaky, friends. xx

As always, please note that I do not have a professional background in the medical field. If I speak in error, it is an honest mistake and I will correct it as soon as I am made aware.















Comments